DIAGNOSTIC PROCEDURES IN HEART DISEASES
Exercise Test (Stress Test)
The exercise test can be applied in two ways.
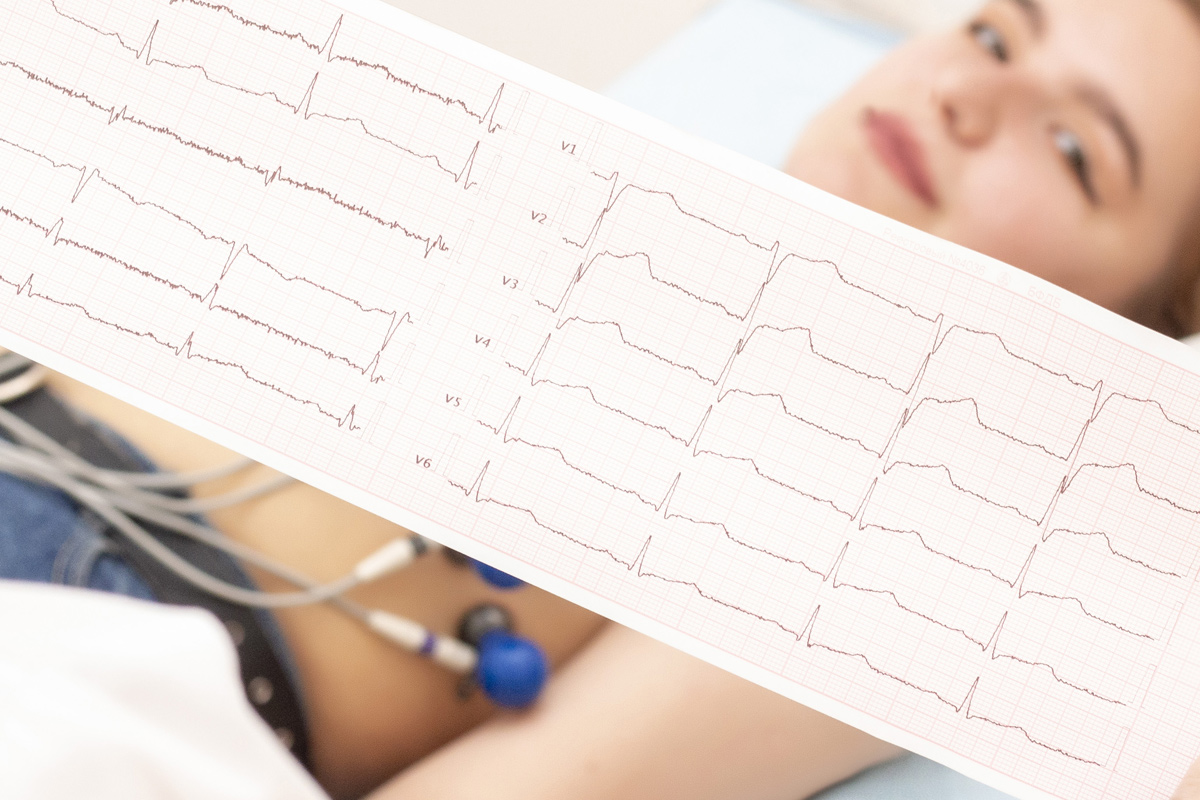
– Exercise ECG (Electrocardiography)
– Stress ECHO (Echocardiogram) (with exertion or medication)
a. Exercise ECG:
Continuous measurement of electrocardiography of the heart is called “exercise test” while the patient suspected of having stenosis of the cardiac vessels walks at a fast pace on the treadmill.
b. Stress Echocardiogram:
An ultrasound examination (ECHO) of the heart is performed before and immediately after the exercise test in some special cases, which increases the accuracy of the diagnosis of heart disease compared to the normal exercise test.
A 4-hour fasting period is required for the exercise test. It is advantageous for patients to come with athletic shoes and tracksuits if possible.
Echocardiography and Color Doppler
The technique that converts the structure of the human heart, the diameters of its chambers, the working capacity of the myocardium, and, in particular, the structure and functions of the heart valves into live images using the ultrasound wave method is called echocardiography (ECHO). No preparation or fasting is required for this test and the entire test can be performed in a short time.
Cardiac Catheterization and Coronary Angiogram
With the cardiac catheterization and coronary angiogram, it is possible to closely observe the structure of the heart, pressures in the heart chambers and large vessels, stenosis, and insufficiencies of the heart valves, and especially stenosis or occlusions of the heart vessels. Thanks to this technology, separate radiological images of each of the heart vessels are taken from different angles. The procedure usually takes between 10 and 20 minutes, and bed rest is required for 4-6 hours after the procedure. It is performed with the help of a catheter that is passed from the femoral artery to the heart under local anesthesia. During cardiac catheterization, the pressures in the heart are measured and at the same time the contractile function of the heart is examined by injecting a dye (contrast substance) into the left heart chamber.
Holter Monitor (Heart Rate or Blood Pressure Holter)
Heart rhythm is monitored and recorded for 24 hours with a device called Holter. This device can be used to diagnose cardiac arrhythmias.
The blood pressure Holter device also records fluctuations in the patient’s blood pressure values for 24 hours, during the day, under real conditions and during sleep.
Electrophysiological Study
It is the most definitive method of diagnosing cardiac arrhythmias. Thanks to this procedure, which is performed with the help of a special catheter passed under local anesthesia from the femoral vein to the heart, the locations of arrhythmias that cause the heart to work too fast (tachycardia) or too slow (bradycardia) are determined by ‘millimetric’ measurements and the ‘map of arrhythmia’ required for definitive treatment is created. This method, which requires very advanced knowledge and technologies, can be applied only in a few centers in Turkey.
Cardiac MRI
It is an imaging technique that can show the structure of the pericardium, heart chambers and valves, myocardium and large arteries coming from the heart, as well as some heart diseases (such as stenosis, vasodilatation, calcinosis) in an extremely simple and harmless way. The processing time is about 15 minutes and requires no prior preparation.
Nuclear Cardiology
a) Myocardial Perfusion Scintigraphy (Thallium Stress Test)
It is a more sensitive method than the exercise test to determine if there is occlusion or stenosis in the vessels supplying the heart. Thallium, a radioactive substance given intravenously, is used to examine the blood supply (or nutrition) to the myocardium is examined at rest and during exercise. A fasting period is required for the test.
b) MUGA: It is the most accurate method of measuring the pumping capacity of the left ventricle. Before the procedure, the red blood cells of the blood are marked with a radioactive substance called technetium. Cardiac function is measured by simultaneous imaging with an ECG scan.