Arteriosclerosis
What is peripheral vascular disease?
Peripheral vascular disease (PVD) is the degeneration of the arterial system in our body due to atherosclerosis. In this degeneration, the interior of the vessel first narrows due to calcinosis and the accumulation of fatty layers on the walls of the vessels, and then with the progression of the disease, complete occlusion occurs.
 What are the causes of PVD and in whom does it occur more frequently?
What are the causes of PVD and in whom does it occur more frequently?
PVD is a disease that usually occurs in advanced age (over 50 years). It occurs more frequently in men than in women. In addition to family history and genetic factors, lifestyle habits such as smoking, lack of exercise, irregular diet, and chronic diseases such as hypertension, hyperlipidemia, diabetes, and kidney failure are factors that increase the incidence.
In which vessels is it most common?
PVD most commonly occurs in the leg vessels of the body. However, the carotid arteries (carotid artery disease), brachial arteries, and visceral organ veins (kidney, intestine, etc.) may also be affected.
What are the symptoms of PVD?
When PVD affects the vessels that supply the organ, there are findings about that organ. It usually occurs in the arteries of the leg and the symptoms vary depending on the degree of narrowing and the location of the occlusions in the leg arteries.
 Common complaints can be listed as follows:
Common complaints can be listed as follows:
• Pain: The pain begins when walking and disappears when resting. It is a cramp-like pain that occurs in the muscles of the affected region due to the undersupply that results from not being able to get enough oxygenated blood to the narrowed area. While the pain of problems in arteries in the upper part of the leg is felt throughout the leg, the problem in vascular occlusion in the knee area is in the region below the knee.
The more severe the occlusion and stenosis, the less exertion the pain causes and the later it subsides. In the advanced stages of the disease, pain at rest without exertion is observed.
Arteriosclerosis
• Wound: depending on advanced undersupply to the legs and feet, wounds may open spontaneously, or a wound opened by a cause such as trauma or a cut may not heal.
• Gangrene: This is the loss of vitality of the limbs when they are undersupplied. Amputation of the gangrenous part is often unavoidable.
Arteriosclerosis
How is PVD diagnosed?
The first step of diagnosis is the examination and the arm and foot pressure ratios. After that, it is necessary to use imaging techniques.
Doppler ultrasound examination of the arteries does not provide precise information about the stage of the disease, but it does provide approximate information about the stage of the disease and the vessels involved.
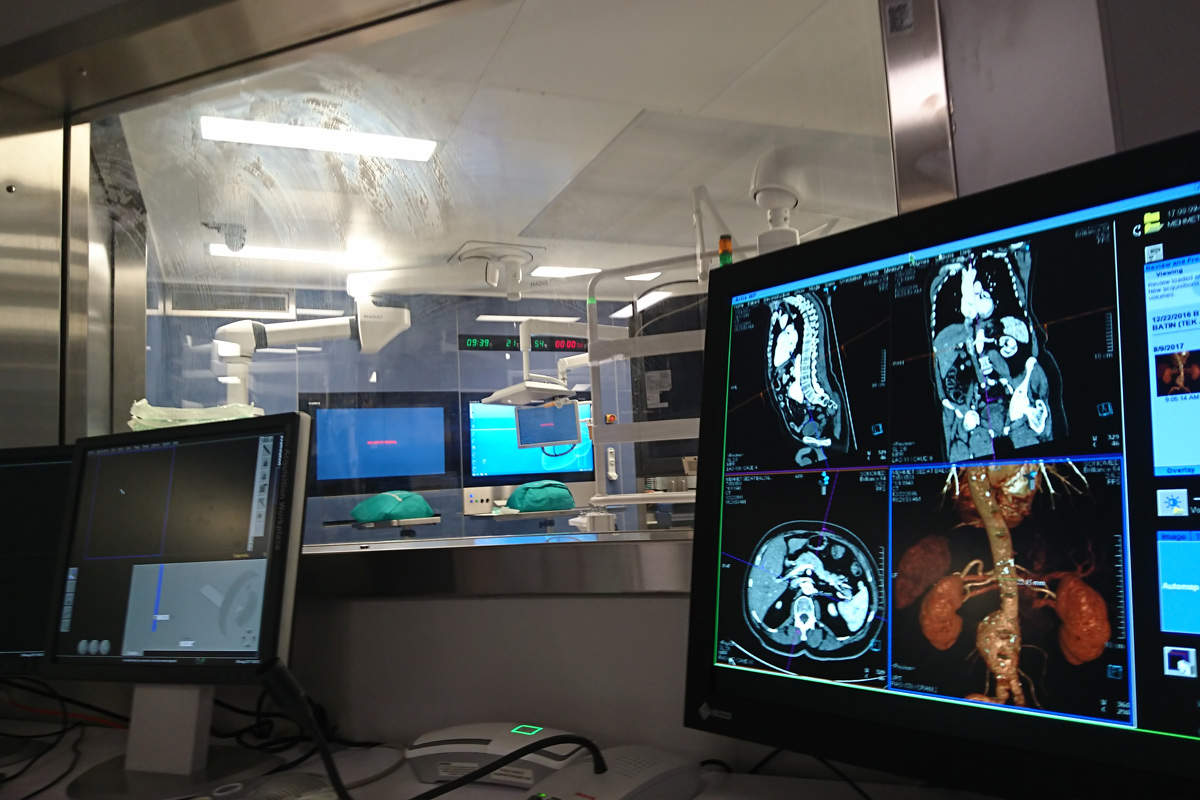
Angiographic diagnostic techniques must be used to make a definitive diagnosis and guide treatment. Magnetic resonance (MR) or computed tomography (CT) angiography can objectively determine the location and degree of stenosis and identify 3D anatomic features.
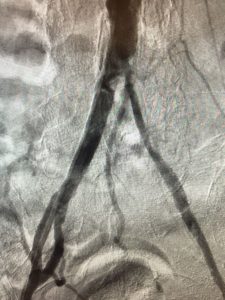
With conventional angiography, both diagnoses can be made and balloon, stent, or other procedures in cases requiring treatment can be performed during one procedure.
Arteriosclerosis
What are the treatment options?
Since the effects differ according to the stage of the disease, the treatment also differs according to the person. Therefore, the treatment of people with PVD should be planned taking into account the patient’s disease, symptoms, limb vitality, and the person’s social expectations.
In cases of pain at rest, gangrene or a non-healing wound in the foot or leg, interventional treatment that increases blood supply is absolutely necessary because of the risk of losing the limb and perhaps life. However, for patients who have no symptoms other than pain when walking, the treatment method should be chosen with consideration of factors such as the patient’s age, social circumstances, and the extent to which his or her life is affected by the disease. For example, for a 50-year-old, active, working patient, surgical treatment may be recommended to treat pain on walking 1 km, whereas for an 80-year-old patient who leaves home 1-2 times a week and has pain on walking 250 meters, medical treatment and follow up may be recommended.
What should a patient with PVD pay attention to?
It is necessary to eliminate all factors that cause the development of the disease. Family factors are inevitable and unchangeable. However, these patients must stop smoking, exercise and lose weight.
People with PVD are recommended to walk at least 3 times a week for 45-60 minutes at an athletic pace. In addition, factors such as hypertension, hyperlipidemia, and diabetes, which play a direct role in the development of PVD, should be adequately controlled.
Even taking these precautions alone will increase the walking distance of patients by 1.5-2 times within 3-6 months.
Arteriosclerosis
Is medication therapy effective in PVD?
There are drug treatments for PVD that have been shown to be effective. In particular, some blood-thinning and procirculatory medications can increase walking distance by up to 2 times within 3-6 months of their use and relieve existing pain at rest.
The most commonly used medication therapy is the anticoagulant medication aspirin and the medication Pletal (cilastazol), which has vasodilator and blood thinning effects.
In PVD, the medications must be used under the supervision of a physician.
What other treatment options are available for PVD?
Interventional treatment methods and surgical treatment methods are used for patients who do not achieve the expected results despite changes in lifestyle and medication therapy.
Interventional treatment methods are procedures that are accompanied by angiography. It is an effective treatment method widely used in the world and in our country.
Treatment is possible with atherectomy (removal of plaques causing vascular occlusion), balloon and stent systems, which are inserted into the area over a fine wire system during the procedure, depending on the location and length of the occlusion or the stenosis. Patients are discharged 6-8 hours after the procedure or the next day, depending on the length and techniques used during the procedure.
Surgical treatment methods are used in cases with very long or complete occlusion where interventional methods cannot be used or in cases of recurrent stenosis after interventional methods.
There are basically two types of surgical techniques: Bypass and plaque removal. In bypass surgery, a new bridge is created before and after the occlusion that causes peripheral vascular disease, either through veins taken from the body or artificial vessels. In this method, blood is directed beyond the occlusion via an alternative new pathway. Plaque removal involves opening the artery in the area where the blockage is located, cleaning the inside, and then repairing the artery.
Arteriosclerosis
Tags: arteriosclerosis, vascular occlusion, Buerger’s disease, balloon, stent, angiography, bypass, artificial vessel, acute vascular occlusion, endovascular, percutaneous intervention, catheter, Reynaud’s syndrome, Reynaud’s disease, gangrene, leg wound